Optimizing COPD Treatment: A Deep Dive into Medications
Introduction
Pharmacologic treatments for COPD are designed to alleviate symptoms, mitigate the likelihood and intensity of exacerbations to enhance health-related quality of life, and exercise tolerance.1 Some common pharmacologic treatments for COPD and their modes of action are outlined in (Table 1).
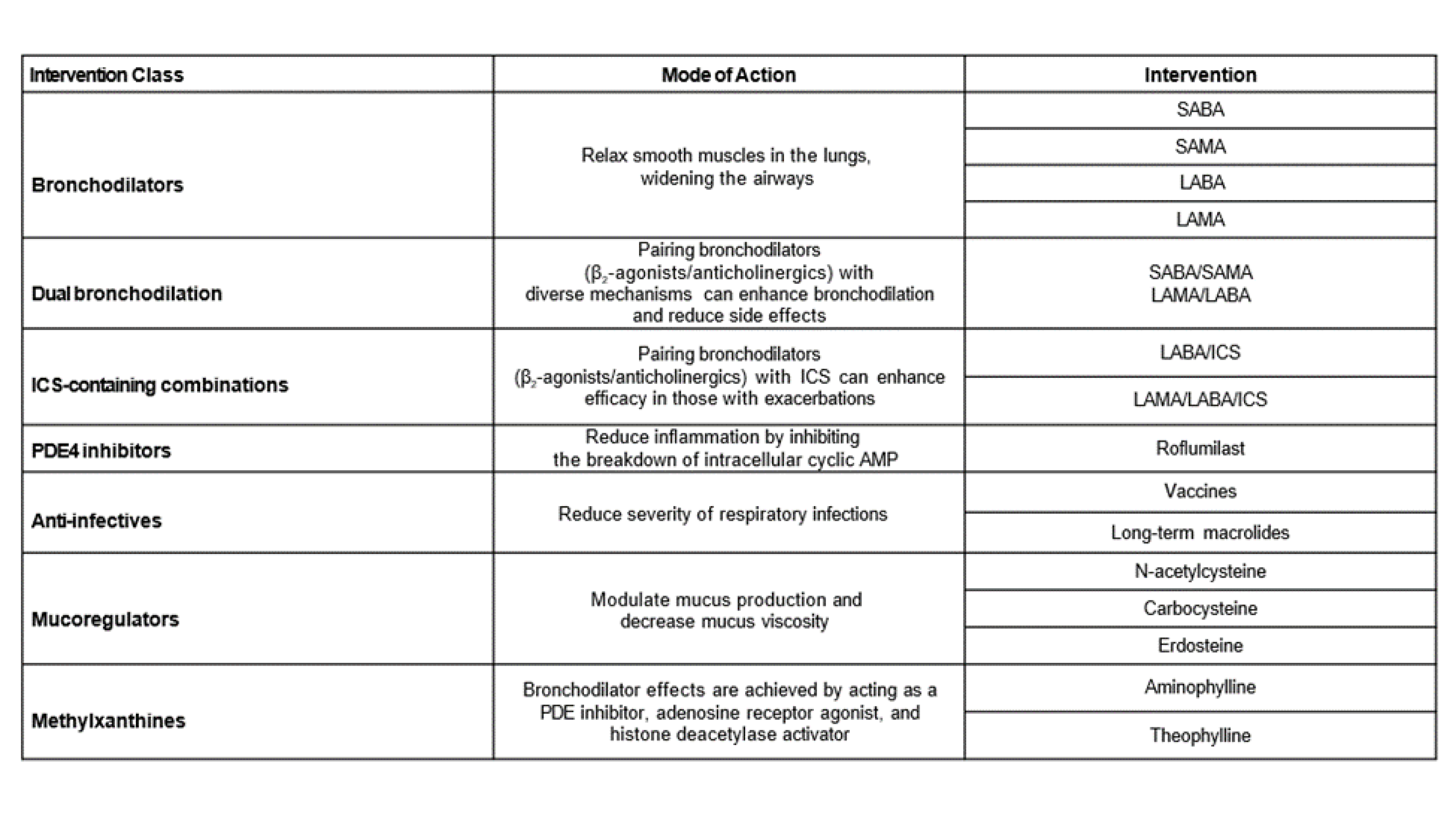
Table 1. Common pharmacologic treatments for COPD1-4
As inhaled therapy plays a central role in COPD treatment, ensuring the proper use of these devices is essential to maximize the benefits while minimizing risks.2 Education and training for both HCPs and patients on the correct use of inhaler devices is crucial.2 Regular follow-up assessments are also vital to ensure the continued effective use of inhaler devices.2
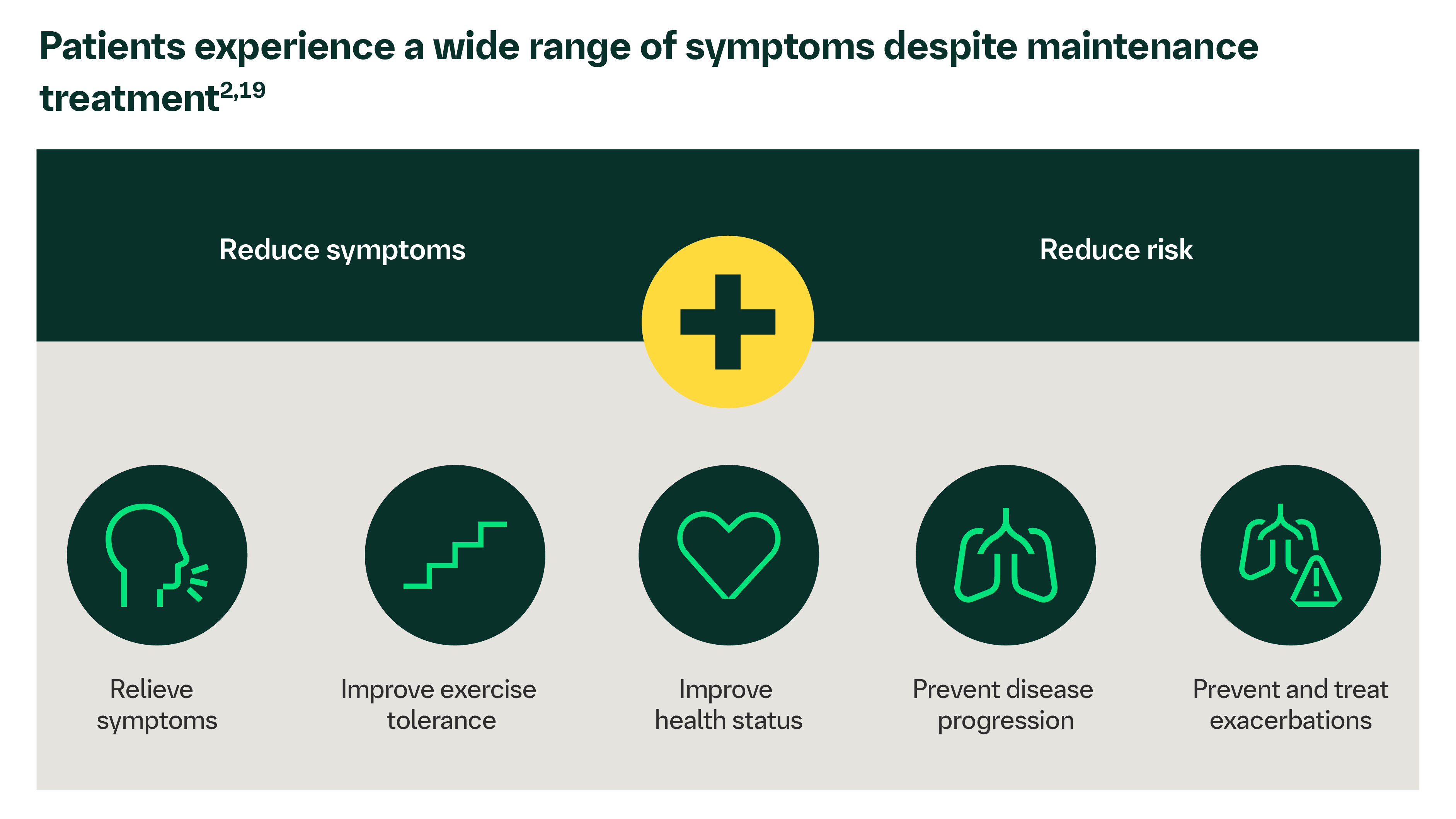
PATIENTS CAN OR MAY HAVE A WIDE RANGE OF SYMPTOMS1
Initial pharmacologic treatment
The GOLD 2024 report recommends different initial pharmacologic treatments for patients with COPD based on the number and severity of symptoms and exacerbations a patient experiences (Figure 1).1 Patients can be split into three groups:

Patients should receive bronchodilator treatment (either short- or long-acting) to alleviate breathlessness. When feasible and within budget, a long-acting bronchodilator is the preferred option, with the exception being patients who experience very occasional breathlessness.1

Patients should initiate treatment with LABA/LAMA unless issues of availability, cost, or side effects arise. While dual bronchodilation is the recommended initial pharmacological choice for patients with COPD in this group, if the patient is unable to receive this, there is no clear preference for one class of long-acting bronchodilator (LABA or LAMA) for initial symptom relief. A patient’s perception of symptom relief can help guide this decision.1

Patients are advised to initiate therapy with LABA/LAMA, unless their blood eos count is ≥300 cells/μL, when the addition of ICS for triple therapy may be considered. The use of LABA/ICS is no longer recommended for patients with COPD. For patients with concomitant asthma, treatment should follow an asthma management approach.1
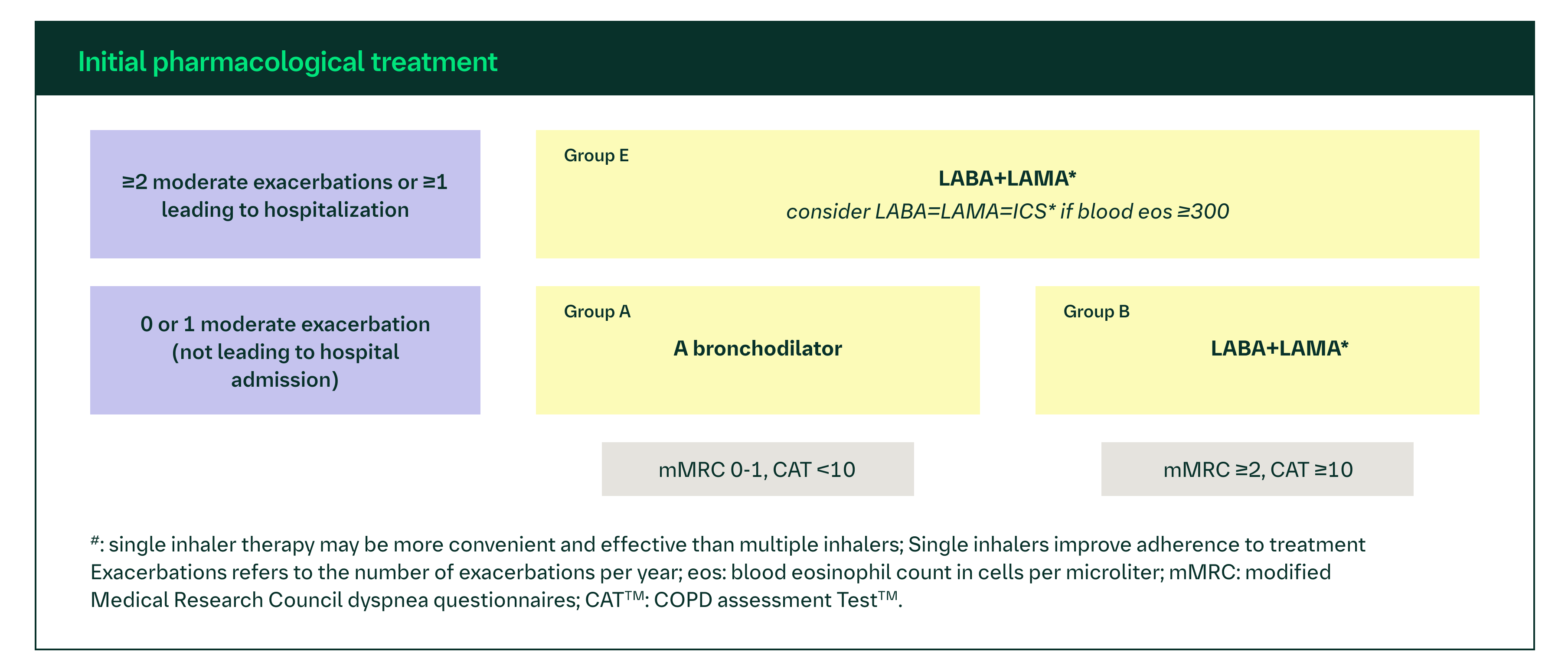
Figure 1. Initial pharmacologic treatment of COPD.1 © 2024 Global Initiative for Chronic Obstructive Lung Disease.
Follow-up pharmacologic treatment
After initial treatment, patients should undergo routine reassessments.1 Follow-up pharmacologic management should be guided by the principles of first review and assess, then adjust if needed.1 The GOLD 2024 report recommends follow-up care is based on addressing two treatable traits: dyspnea and the frequency of exacerbations (Figure 2).1,2
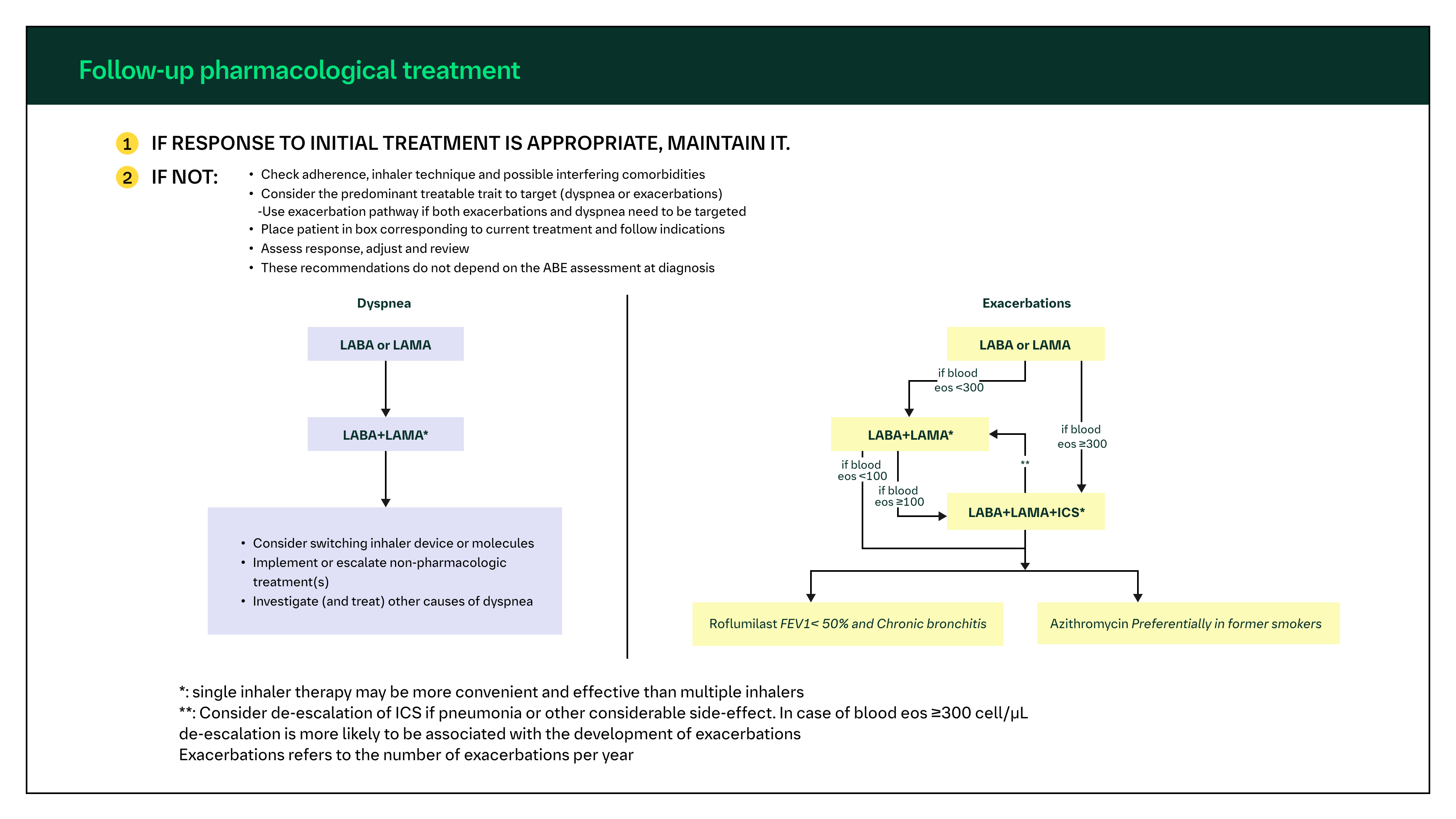
Figure 2. Follow-up pharmacologic treatment.1 © 2024 Global Initiative for Chronic Obstructive Lung Disease.
GOLD 2024 recommended the use of LABA, LAMA, or LABA/LAMA combinations in patients with dyspnea or exacerbations, except in those with exacerbations whose blood eosinophil is ≥300 cells/μL, in which case LABA/LAMA/ICS may be considered. In cases of ongoing exacerbations despite LABA/LAMA/ICS therapy or eos counts <100 cells/μL, roflumilast or a macrolide may also be considered.2
Patients whose pharmacologic treatment undergoes modification require close monitoring.2 It is reasonable to continue LABA/ICS for well-controlled patients without asthma features. However, if persistent dyspnea is observed, switching to LABA/LAMA (with or without ICS) can be considered in case of further exacerbations.2 It is important to note that the use of ICS is discouraged in patients with a history of recurrent pneumonia, prior mycobacterial infections, or an eosinophil count <100 cells/μL, as there are well-documented adverse effects associated with its use.1
Key Takeaways

Alleviate COPD symptoms and reduce exacerbation risk to improve quality of life and exercise tolerance.1,2

Proper use is essential, necessitating education and regular follow-up assessments.2

Tailored based on exacerbation frequency and severity.1

Targets treatable traits, emphasizing dyspnea and exacerbation management.1,2

Close observation and adjustments based on patient responses and specific circumstances.1,2

A key focus throughout the treatment process.1,2
Abbreviations:
-
CATTM, COPD Assessment TestTM; COPD, chronic obstructive lung disease; eos: eosinophils; FEV1: forced expiratory volume in 1 second; GOLD, Global Initiative for Chronic Obstructive Lung Disease; ICS, inhaled corticosteroid; LABA, long-acting β2-agonist; LAMA: long-acting muscarinic antagonist; mMRC, modified Medical Research Council dyspnea questionnaire.
References:
-
Global Initiative for Chronic Obstructive Lung Disease 2024. Available from: https://goldcopd.org. Last accessed November 2023.
-
Agustí A, et al. Am J Respir Crit Care Med 2023;207:819–837.
-
Aaron SD. Eur Respir J 2017;50:1701465.
-
Barnes PJ. Pharmaceuticals 2010;3:725–747.